By Rowan Walrath, managing editor
Just over a year before he graduated, Brandon, who wished to keep his last name private, found his roommate dead on the bathroom floor. After only one month of knowing his fellow Northeastern student, Brandon was faced with reporting his suicide, moving out of the tainted apartment and going to emergency counseling.
“They [at counseling] were obviously really accommodating, probably because housing was pushing them,” Brandon said. “That worked perfectly well. It was easy enough to get help in an emergency situation.”
However, though the emergency sessions that University Health and Counseling Services (UHCS) provided were useful, they didn’t last beyond a few weeks. A year later, when Brandon found himself experiencing symptoms of depression and anxiety that likely stemmed from post-traumatic stress disorder (PTSD), UHCS was of no help at all.
“I called them probably mid-January, right about the start of the semester, and they were booked up for like two weeks,” Brandon said. “They made me an appointment for two weeks later, at which point it was snowed out.”
Another two weeks of a brutal Boston winter. Another snowed-out appointment. Brandon rescheduled for an appointment another two weeks from that time. Finally, a full six weeks after his initial call, Brandon went in to see a counselor – and she failed to show up. Although UHCS staff told Brandon someone would call him to reschedule his appointment, weeks passed, then months, before he finally gave up. No one was going to call.
“College counseling centers have been a major issue with access to mental health care,” Jeffrey Axelbank, a licensed psychologist practicing in Highland Park, N.J., said. “That’s across the country. College counseling centers are being overwhelmed by the demand for their services. You’ll go […] and there’ll be a three-week or six-week waiting period, and by that time, the semester’s over. That’s a national problem.”
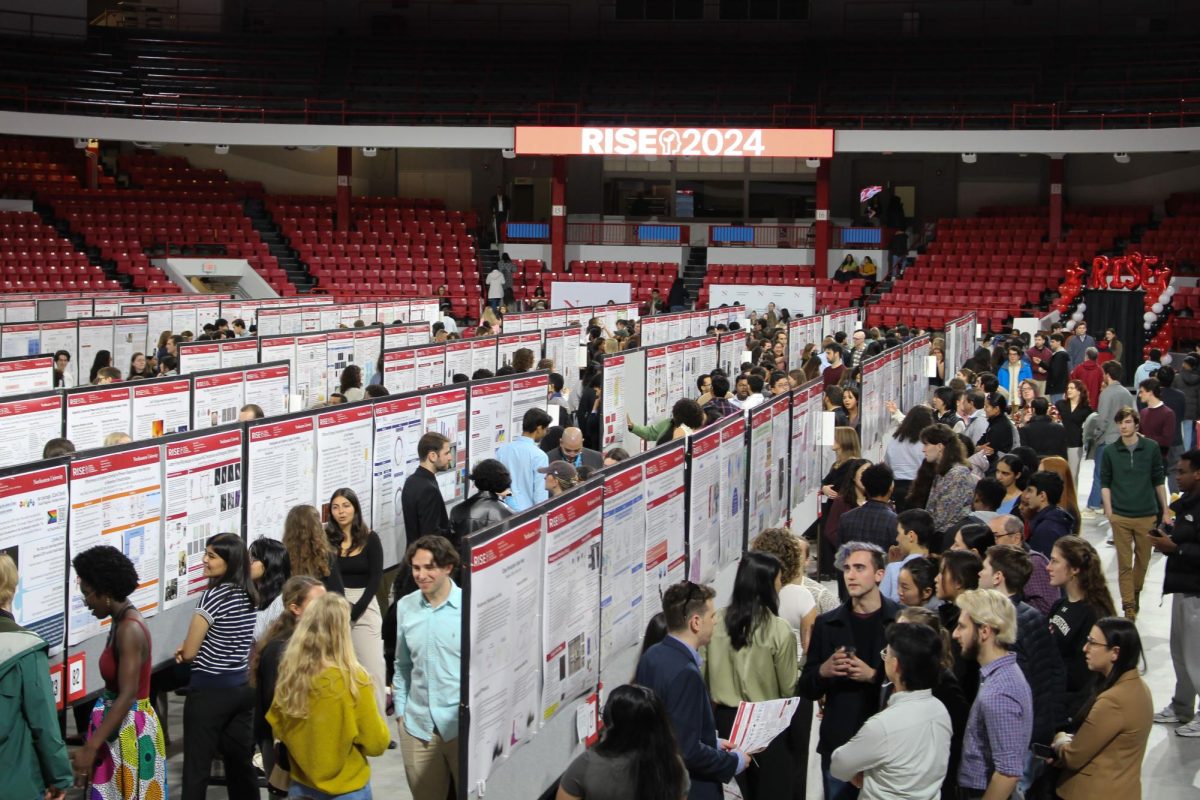
At Northeastern, UHCS provides only a handful of mental health counselors for more than 16,000 undergraduate students.
“UHCS currently has 14 behavioral health care providers in addition to the doctors, nurse practitioners, physician assistants and nurses on the medical team,” Associate Dean for Student Affairs and Dean of Students Madeleine Estabrook said.
According to Estabrook, students can be seen on the same day for urgent needs, while scheduled behavioral health appointments are either 30 minutes or an hour long. The university’s model is based on short-term therapy.
UHCS has an external referral process to alleviate the pressure on those 14 full-time behavioral health care providers. According to Estabrook, a referral coordinator gives those students who request them the names of clinicians who are nearby and accepting new patients.
However, the process does not always go as smoothly as promised. Kathryn Schmitt, a third-year psychology student at Northeastern, has been diagnosed with depression and anxiety. After she decided she needed to see a therapist more frequently than UHCS could allow for, she asked for recommendations. Of the two to three local clinicians she called, two picked up, and Schmitt successfully scheduled an appointment with one of them.
“I went to one session with her and […] my schedule was so busy, I called her to cancel, and she never called me back,” Schmitt said.
That cancellation call was the first of many calls Schmitt made to the therapist in an attempt to reach her, but to no avail. The woman never called back.
“I think I’m picky about who else I see,” Schmitt said. “I was put off by that experience.”
Stephanie, a third-year psychology major with a minor in behavioral neuroscience at Northeastern who wished to keep her last name private, had a similar experience with UHCS’s referral system.
“I was given referrals and I was contacting referrals, and none of them could accommodate me while I was available,” Stephanie said.
Stephanie’s schedule wasn’t particularly difficult to accommodate. She had no classes on Fridays, and her late afternoons were also free to potential psychiatric appointments.
“I ended up not making any kind of appointment,” Stephanie said.
However, Stephanie’s therapist at UHCS has found a way to get her in. She said that occasionally, her therapist schedules her during emergency slots, 20 to 30-minute windows for walk-in appointments designed to help students who need emergency care.
Of course, this practice in itself is concerning. Stephanie is not an emergency patient. There may be another student having a panic attack in UHCS’s waiting room while Stephanie occupies the time and attention of the on-call clinician.
Where college counseling centers like UHCS might fail, other organizations in the area try to help students. The National Alliance on Mental Illness (NAMI) Massachusetts chapter provides resources to patients who are finding difficulty connecting to local practitioners.
“Our helpline is designed to help people get connected to local resources who help them find treatment or other issues that tend to crop up with mental health issues like difficulties finding housing, securing employment, things like that,” Megan Wiechnik, a resource helpline coordinator at NAMI, said.
Barriers to accessing mental health services that Wiechnik’s clients come across are often intervening legal issues or the criminal justice system. However, the biggest barriers, she said, are the scarcity of providers who are easy to connect with and the stigma people associate with mental illness.
“I can tell you that it is really hard to find a provider that is a good fit,” Wiechnik said. “And we’re talking about a very personal relationship that you build, especially with a therapist and a psychiatrist. The medications that they prescribe affect a really sensitive part of the body – the brain – and it’s really difficult to find someone. You want someone you’re comfortable with.”
Wiechnik is also a recent Northeastern graduate. After working a co-op with NAMI, she went on to become a full-time employee when she left the university in 2012. During her time at Northeastern, Wiechnik utilized resources at UHCS, although she believes they could be farther-reaching.
“I definitely think they could be doing a lot more,” Wiechnik said. “A lot of it comes down to the stigma where even though services are there, kids don’t feel comfortable using them or they don’t want to be seen walking into the health center or whatever.”
Unfortunately, even for those who overcome the mental health stigma that some have called a national crisis, students and others will likely still have difficulty finding a clinician who can meet their needs. An October 2014 study conducted by Harvard Medical School researchers found that access to mental health care is very limited. In the study, researchers posed as patients with depression who would offer to pay using BlueCross BlueShield, Medicare or out-of-pocket.
Of the 360 psychologists they called, an estimated 15 percent of the clinics were not accepting new patients, 23 percent of psychiatrists did not return phone calls and 16 percent of the phone numbers listed in insurers’ databases were inaccurate. Researchers were completely unable to schedule any type of appointment 75 percent of the time.
“I think in Boston… despite the fact that there are so many doctors per capita, the demand is high enough that […] people feel like they don’t even need to return phone calls,” J. Wesley Boyd, a professor of psychiatry at Harvard Medical School, staff psychiatrist at Cambridge Health Alliance (CHA) and the study’s lead researcher, said.
BlueCross BlueShield did not respond to request for comment.
According to Axelbank, speaking for mental health professionals, insurance companies end up limiting access to mental health care by decreasing the pay professionals receive for their services.
“From my end, I know that there’s a question for many therapists as to whether to be in network or out of network,” Axelbank said. “The trade-off is: If you’re in an insurance network, you have a ready-made pool of potential clients […] you tend to get more referrals more easily. The downside, from our point of view, is that they pay less, sometimes significantly less, than what would be the paying rate otherwise.”
That disparity in salary also leads to a disincentive for students to go into psychiatry, according to Boyd.
“Psychiatry pays less, psychiatrists are nearly at the bottom of all doctors […] so medical students are less likely to go into psychiatry,” Boyd said.
The number of people going into the field of psychology is on the decline despite a growing need for psychological services. According to Axelbank, insurance agencies have a great deal of influence here, even causing many people to avoid the profession altogether.
“If you take a step back and look at the whole system, part of the reason why there’s a shortage of therapists is it’s become less viable to have a practice because of these insurance issues,” Axelbank said. “So less people are going to graduate school to get trained, which means less people are graduating, which means less people are available.”
According to the American Psychological Association (APA), it is estimated that approximately 1.5 million undergraduate students complete an introductory or general psychology course each year. However, only 25 percent of psychology baccalaureate recipients continue on to graduate study in psychology – approximately 4 percent to 6 percent doctoral, 20 percent to 22 percent master’s.
“Also, medical students probably see psychiatry as ‘Hey, I have to get authorization from the insurance company to do what I want with my patients,’” Boyd said. “Only psychiatry has that last requirement.”
Axelbank agrees with Boyd on this last point: Insurance companies serve as a barrier between clinicians and patients, potentially preventing patients from getting the care they deserve.
“Insurance companies are really, in my mind, sort of strangling the access,” Axelbank said. “It’s a log jam in the process of getting people the help they need. Other obstacles about this in particular, getting mental health care, is that people don’t like to admit they need it, there’s a cultural issue […] but I think that a major issue is the insurance companies kind of narrowing the access.”
In 2008, a supplemented version of the 1996 Mental Health Parity Act, this time called the Mental Health Parity and Addiction Equity Act (MHPAEA), went into effect. It was designed to prevent insurance companies from making a distinction between medical and behavioral health care. According to the United States Department of Labor website, financial requirements and treatment limitations must apply equally to mental health or substance use disorders and physical ailments.
On paper, this is supposed to make it impossible to discriminate against people with behavioral health issues. In practice, however, insurance companies find creative ways to get around MHPAEA.
“One of the things we deal with all the time is they don’t say you’re limited to 20 sessions a year, but after 20 sessions, they’ll call or write the therapist and say, ‘If you want to have more sessions, you have to fill out this paperwork,’ or all kind of hoops you have to jump through,” Axelbank said.
In 2000, an official Privacy Rule was added to the 1996 Health Insurance Portability and Accountability Act (HIPAA). The rule, last modified in 2002, establishes national standards to protect individuals’ medical records and other personal health information, according to the United States Department of Health and Human Services website. It also gives patients some control over their health information, including requiring authorization to disclose information and giving patients rights to examine, obtain and correct a copy of their health records.
However, some of the language within the law itself allows another loophole for insurance companies to slip through.
“One of the things that the law says is that the insurance [needs the] minimum necessary information to process a claim,” Axelbank said. “That’s a pretty strong protection for patients… the problem is that the definition of what’s minimum [and] necessary is not specified in the law.”
Axelbank said in his own practice, he has had to deal with insurance agents asking particularly intrusive questions about his patients. A while back, he was treating a woman who had been sexually abused by her father and suffered PTSD as a result. After a certain number of sessions, the agent asked her for more information to deem whether or not the woman was qualified to receive further treatment – including what exactly had caused her trauma.
“You have this ethical quandary as a therapist,” Axelbank said. “Do you reveal this private information and maybe jeopardize your patient’s confidentiality […] or do you stick by your ethical standards and say, ‘No, I’m not going to reveal this […]’ and maybe not get their sessions authorized? It’s a catch-22.”
Allen Weg, a licensed psychologist practicing in East Brunswick, N.J., believes the only way to change the current situation is to teach patients how to fight back against their insurance companies, to smash the barriers they erect.
“We try to educate our consumers,” Weg said. “Somebody will say to me, it’s really hard for me to continue to come see you, but I’ve seen people from the list from [my insurer]. I say to them, well, you know, try to go down the list and ask these particular kinds of questions […]Then you go back to your insurance company and say, look, you gave me X number of people and… they do not do these kinds of therapy […] This guy is out of network, and I want you to help me pay for this because you’re my insurance company.”
Weg’s vision sees a joint movement by psychiatric patients across the country to force their insurance companies to fully provide for them.
“If enough people did that and held their insurance companies accountable, things would actually change,” Weg said. “It would take a great amount of organized effort.”
Brandon never did find a counselor to see on a regular basis, either through UHCS or externally. Instead, he ended up avoiding the system altogether and taking to the Internet for online therapeutic alternatives.
“There are some sort of software cognitive behavioral therapy things,” Brandon said. “I don’t think it’s as useful as going to see someone would have been, and you have to be fairly sure of what the issue is. I think it worked out okay for me, but it would have worked out better had I actually been able to talk to someone first.”
Photo by Robert Smith